An endodontist case report. MicroEndodontic. Case Study Number 505026 Twenty five years old patient presenting with an abscessed maxillary molar.
To Save or Not To Save? That Was the Question. A Seven Years Post Endodontic Treatment Outcome Follow Up
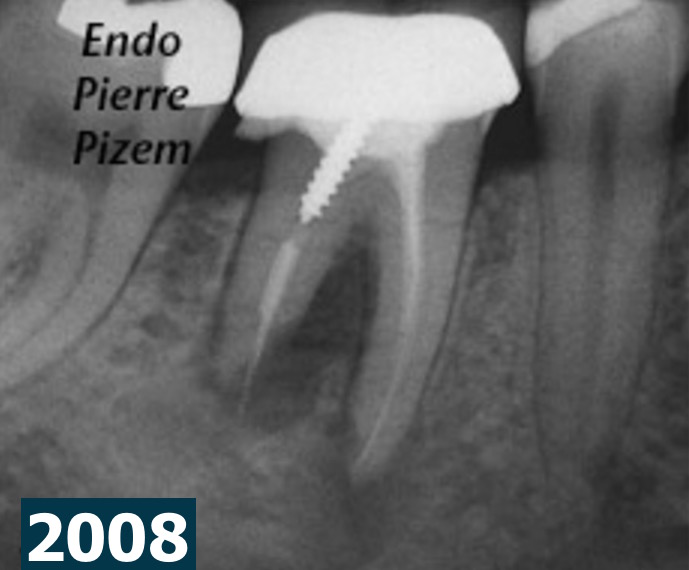
Case Study Number 368745 Patient was told seven years ago to remove lower right premolar and replace this tooth by an implant supported
Good Prognosis is in the eye of the beholder
Case Study Number 430646 External root resorption associated with chronic apical periodontitis altered the shape and position