
Calcified Canals. Case Study Number 487445
Clinical examination: Sinus tract, mobility: 0, deciduous amalgam restoration.
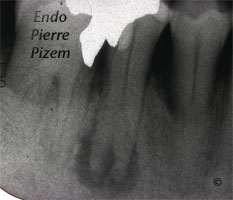
Radiographic examination: Alveolar bone with circumscribed lucency, apical root canal split, hypertaurodontism (bull’s tooth), apical root canal split branches not visible on X ray dental film, hypercementosis
Diagnosis: pulpal necrosis with chronic periapical infection,
Etiology: marginal leakage, caries
Root canal procedure:
First appointment: gaining access to the split, locating entries, shaping and cleaning apical root canal branches inserting intracanal medication for 8 days.
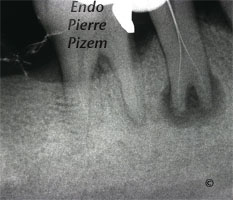
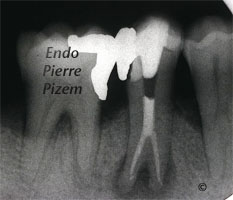
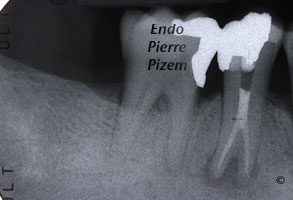
Second appointment: intracanal medication retrieval, copious CHX 2% irrigation, drying canals and permanent root canal obturation with Pulp Canal Sealer and gutta percha (lateral and vertical condensation).
In that specific case, microscope was most helpful during all the following steps necessary to insure a better prognosis for this patient:
1) Locating and gaining access to buccal and lingual root canal entries (apical split was clearly visible under magnified observation)
2) Striving to find a third branch in apical split minimizing the chances of omitting an untreated canal
3) Aiming at the right root canal orifice when:
- Inserting the two first endodontic files to confirm canal lengths
- inserting a file sequence to shape and clean each canal
- Positioning irrigating syringe needle tip and calcium hydroxide syringe tip toward the right canal entry
- Inserting absorbent paper points in both canals when drying canals
- Inserting master, accessory gutta percha cones and finger plugger when doing final obturation with lateral and vertical condensation
4) Checking for pulpal tissue remnants prior to final obturation to minimise the chances of pushing them back into the apical area

Leave a Reply