In daily clinical practice, even by having thorough knowledge of how and where to search for MB2, there are some cases where the microscope magnification alone does not provide enough information on positional relationship between the different root canal entries. This is when the Dental Cone-beam Computed Tomography comes into play.
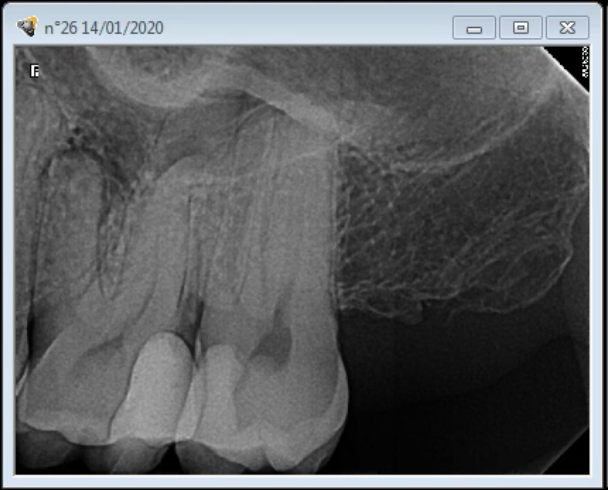
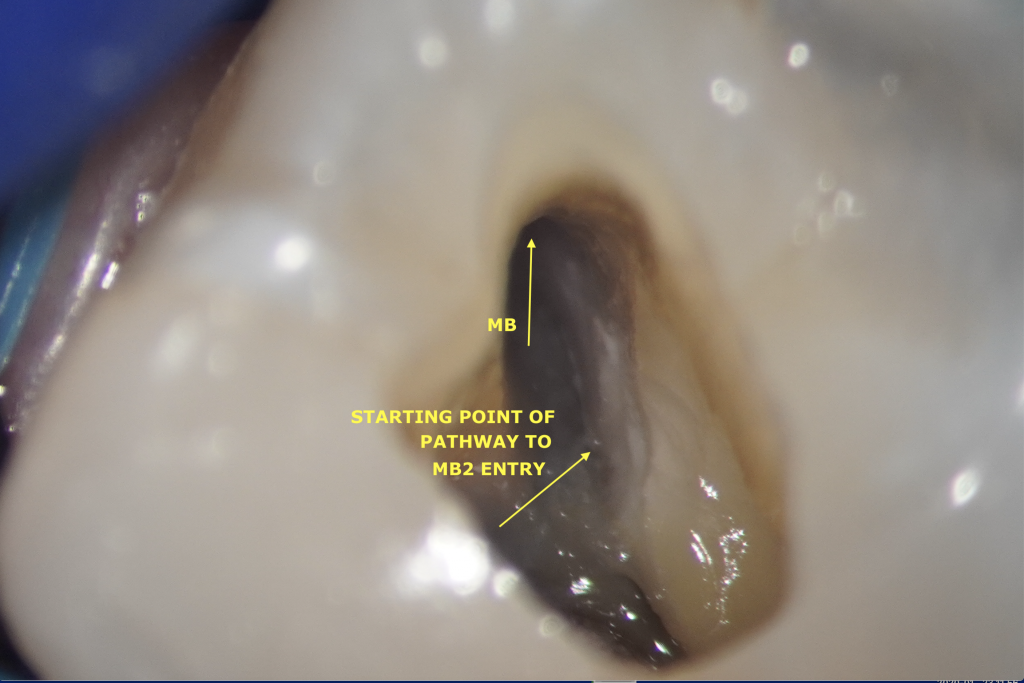
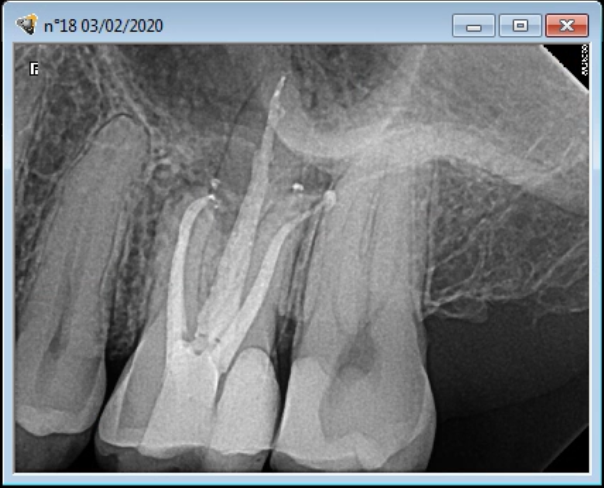
Patient’s first setting was an emergency one. MB, DB and P have been shaped and filled with interim ca(OH)2. Nevertheless, even after some troughing, the MB2 canal entry was impossible to find even under high magnification (Figure 1). In order to avoid the risk of tooth perforation during the troughing preparation, patient has been rescheduled for a Dental Cone-beam Computed Tomography that would confirm that there is indeed an MB2 and were we should be looking for it.

First instruments in MB, DB and P (Mani K files) 
Interim Calcium Hydroxide with Barium Sulfate dressing. Metapaste from Meta Biomed
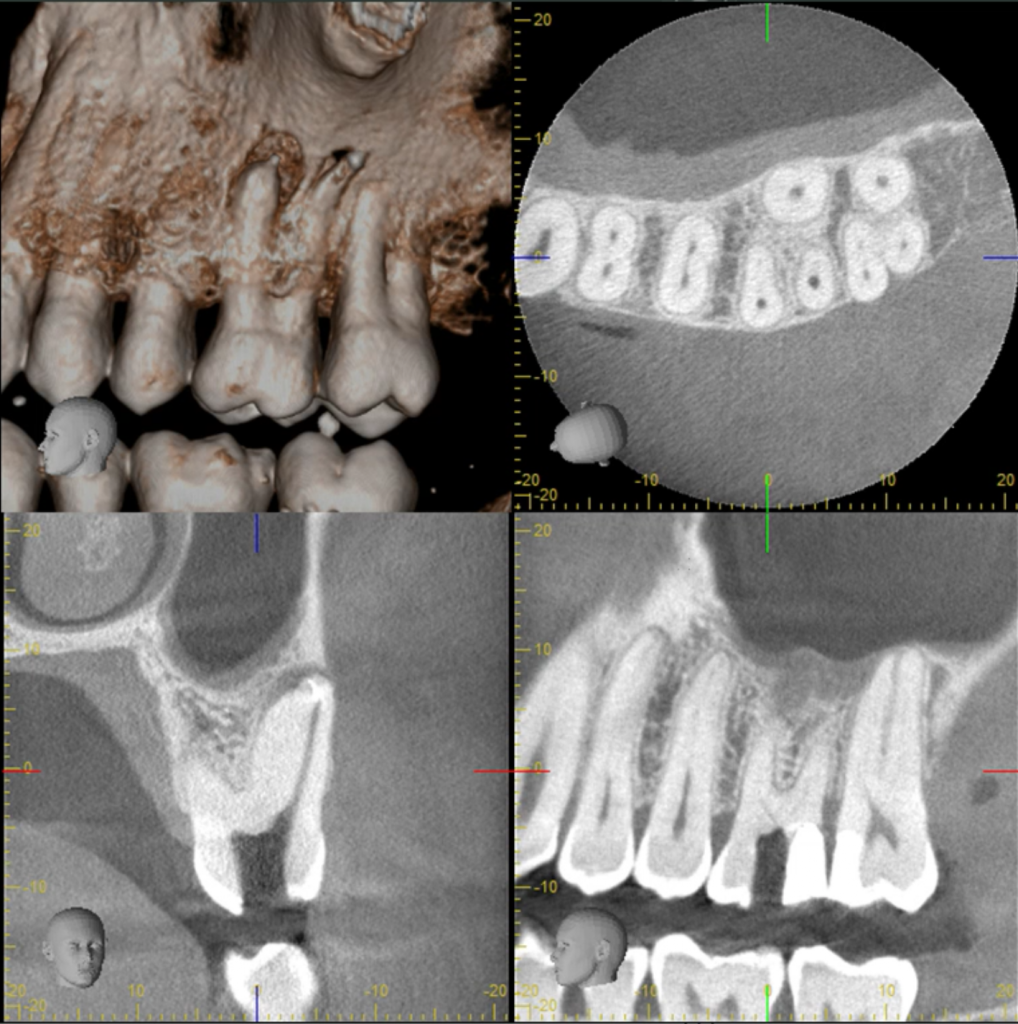
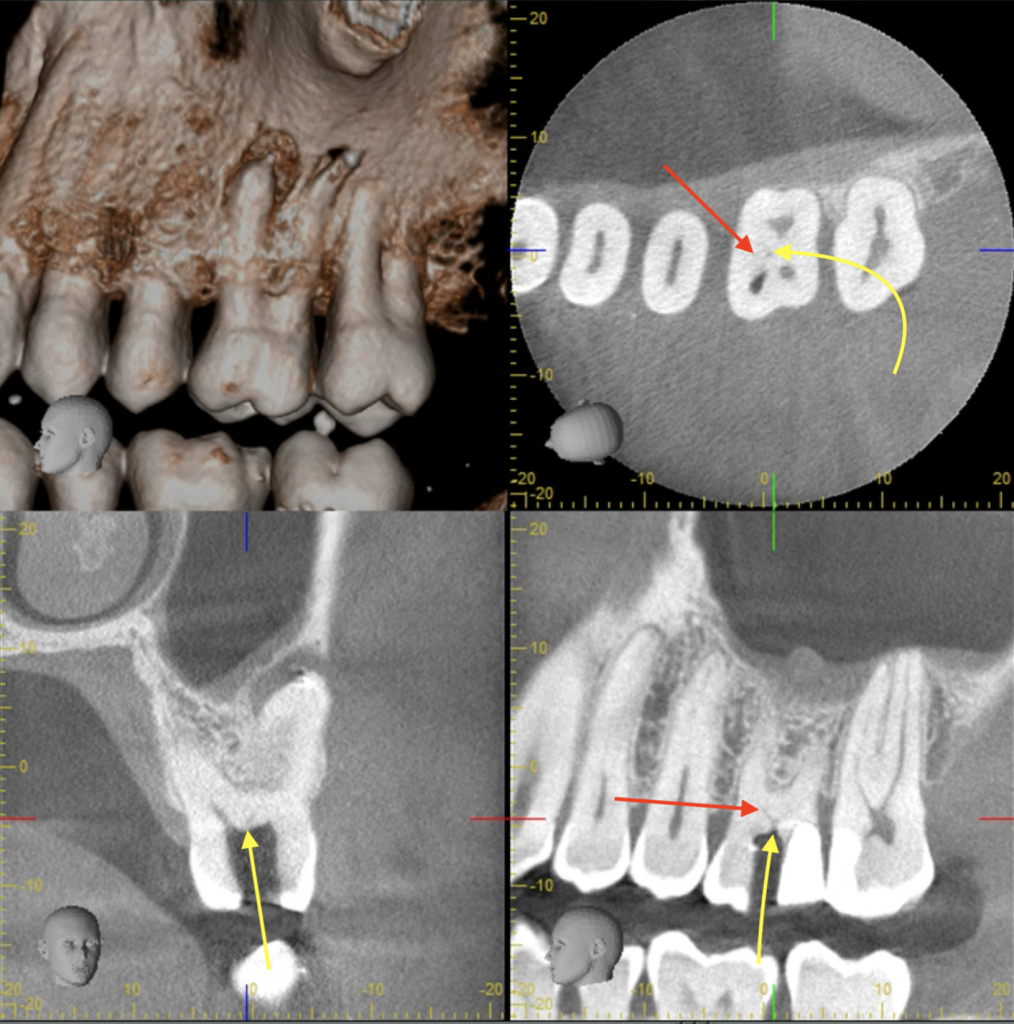
A small volume CBCT Scan has been taken during the second appointment and, as it could be expected, the detailed three-dimensional (3D) observation of the tooth forms and shapes with computed tomography (CT) has been critical in telling where to start troughing (see yellow arrows on Figures 1 and 2 and on 3D scan slices) and where to finish. (red arrows). Once accurate location of MB2 has been obtained, it took 30 minutes troughing to predictably locate and treat it.

MB2 Confirmation with 3D Scan 
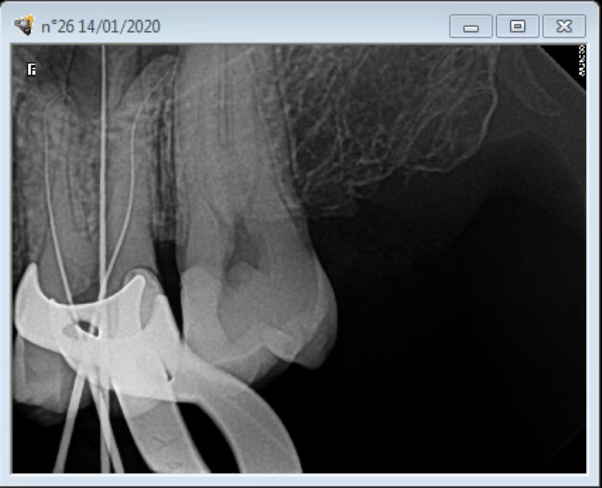
Estimated location of MB2 entry
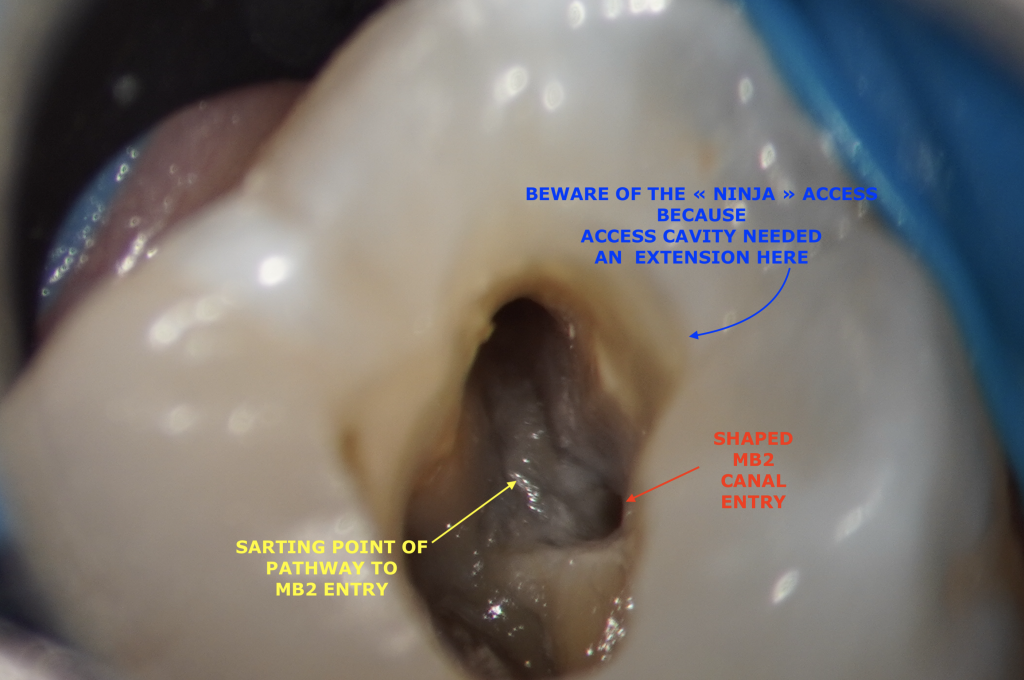
Furthermore, in this case, reaching MB2 entry would have been impossible without adding an extension to the initial access cavity. It is the location of the MB2, which, in fact has been given by the CBCT that determined the amount of extension required to reach that goal.

Figure 1 
Figure 2
It may not be required for all the teeth to be prepared with TEAC (Traditional Access) to detect the MB2 canals. However, a « Ninja » access (or Point Endodontic Cavity Access) would most certainly not have been a wise choice here. Tooth was both necrotic and symptomatic, missing that MB2 with its own portal of exit would have led to a catastrophic failure of this root canal treatment procedure.

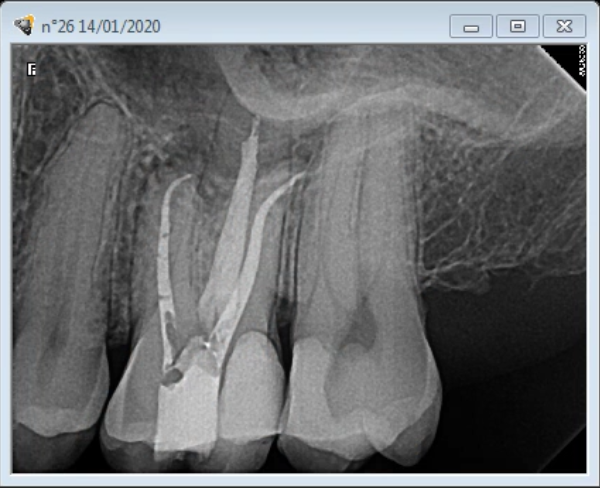
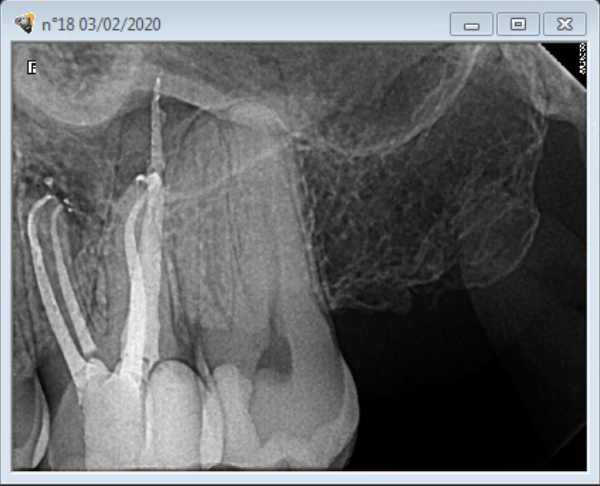
Final Obturation displaying MB2 
Final obturation
The above case is an example of what a combination of both the microscope and the CBCT can help us accomplish. These technologies do represent huge assets in increasing the success rate of endodontic therapy.

Leave a Reply